Plenary - 05: DEVELOPMENT AND IMPLEMENTATION OF A NATIONAL QUALITY IMPROVEMENT SKILLS CURRICULUM FOR UROLOGY RESIDENTS IN THE UNITED KINGDOM: A PROSPECTIVE MULTI-METHOD, MULTI-CENTER STUDY
Nick Sevdalis, PhD, Elena Pallari, MSc, Zarnie Khadjesari, PhD, James Green, FRCS, LLM; King's College London
Background: Improving quality of surgical care is a global priority. Developing effective, evidence-based curricula that teach residents quality improvement (QI) skills can increase capability within surgery to effectively improve services. We report the early design, validation and proof-of concept testing of a novel QI skills curriculum for urology residents in the UK.
Methods: We sought to develop and evidence-based and user-led QI curriculum. We took a multi-method, multi-center approach. We conducted an ‘umbrella review’ of evidence (i.e., review of reviews) on QI curricula – to cover topic areas taught; and curriculum delivery methods (Phase-1). Based on the review, we developed an introductory half-day draft QI curriculum (Phase-2). We submitted the curriculum to review by a senior Steering Committee, consisting of urologists (Attendings & Residents), experts in QI and medical education and patients (Phase-3). We delivered the curriculum to a cohort of urology residents and tested its feasibility, evaluability (through the Kirkpatrick framework for educational interventions) and implementability (Phase-4).
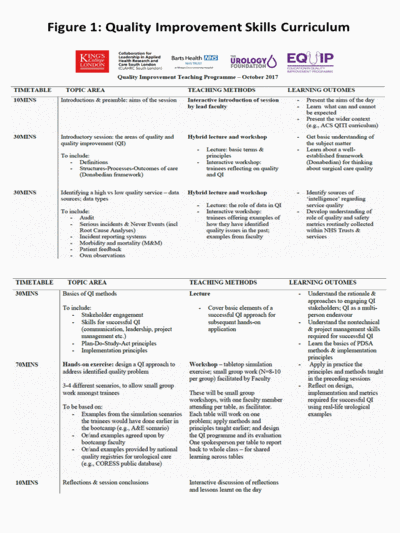
Results: Phase-1: 6 relevant systematic reviews were identified of 4,332 search hits. Most curricula were developed and evaluated in the USA; used mixed teaching methods (incl. didactic, workshops, QI exercises & self-reflection); and introduced core QI techniques (e.g., Plan-Do-Study-Act). Phase-2: based on the review, we developed a draft half-day curriculum (Table 1). Phase-3: our Senior Steering Committee clinical, educational and patient experts judged the curriculum to represent state-of-the-art in QI training and to be relevant to urology residents. The Committee recommended that we incorporate stronger patient and public involvement element in the training; this revision was made. Phase-4: the curriculum was delivered to a cohort of 48 urology residents as part of an annual national urologic surgery bootcamp (Leeds, UK; October 2017). The delivery was feasible; the curriculum fully implementable; and a knowledge-skills-attitudes evaluation approach, driven by the Kirkpatrick framework, was found feasible and effective.
Conclusion: We have developed a QI skills curriculum for urology residents at proof-of-concept level. The content, delivery and evaluation of the curriculum are feasible and relevant to end-users. Further inputs are currently sought from urology program directors and residents across the UK – for UK-wide regular delivery.