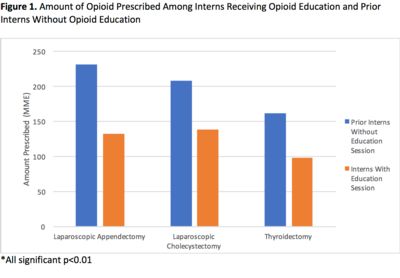
Plenary - 06: THE IMPACT OF A CURRICULUM ON OPIOID PRESCRIBING FOR NOVICE SURGICAL TRAINEES
Alexander S Chiu, MD, Samantha Ahle, MD, Raymond A Jean, MD, Peter S Yoo, MD, Kevin Y Pei, MD; Yale School of Medicine
Introduction: Over-prescription of postoperative opioids has contributed to the current opioid epidemic in the United States. Surgical residents are commonly tasked with prescribing postoperative analgesia, yet most lack formal training in this area. We evaluated the impact of a curriculum for new surgical interns on their comfort in prescribing opioids and the amount prescribed.
Methods: An educational program was developed for surgical interns at a tertiary, academic hospital. The session, provided prior to the start of intern year, covered basic opioid pharmacology, recommended postoperative dosing, and management of narcotic overdoses. A pre-intervention survey assessed prior opioid education experience and comfort level prescribing opioids, and a post-intervention survey evaluated new comfort levels prescribing opioids.
To evaluate the impact on prescribing habits, postoperative opioid prescriptions of interns were compared to the prescriptions of the previous year's interns, who had not received the curriculum. Prescriptions from each group's first two months were compared for the three most common outpatient surgeries: laparoscopic appendectomy, laparoscopic cholecystectomy, and thyroidectomy. Prescriptions were converted into Morphine Milligram Equivalents (MME) to compare across different medications.
Results: The curriculum was provided to 31 interns, with a completion rate of 81% (25) for the pre-survey and 74% (23) for the post-survey. The majority (92%) of interns reported never receiving any prior opioid education, and none had training specifically regarding postoperative opioid prescribing. Only 20% of interns felt comfortable prescribing opioids prior to the education session. After the session, over 90% stated that they felt more comfortable prescribing opioids. Topics reported to be most useful included multimodal analgesia methods, opioid dosing recommendations, and systems based practice information.
Overall, the average amount of opioid prescribed postoperatively was 37% less among interns who received the educational session (127.0MME) compared to historical control that did not receive education (201.6MME, p<0.01). This trend was significant for all three operations studied (Figure 1).
Conclusion: Most incoming surgical residents lack training on, and feel uncomfortable, prescribing opioids. A dedicated curriculum increased comfort in prescribing opioids and significantly decreased the amount prescribed.