PS9-01: SIMULATION-BASED LAPAROSCOPIC ULTRASOUND CURRICULUM IMPROVES SURGICAL RESIDENTSâ SKILLS AND CONFIDENCE
Tetsuya Nakazato, MD, PhD, Mark S Talamonti, MD, Kristine Kuchta, BS, Michael B Ujiki, MD, Stephen P Haggerty; Grainger Center for Simulation and Innovation, NorthShore University HealthSystem
INTRODUCTION: Laparoscopic ultrasound (LUS) is an important tool for minimally invasive surgeons. However, surgical trainees have limited and variable exposure during their rotations. Therefore, we developed a simulation-based LUS curriculum consisting of didactic instruction, mentoring and practice. The aim of this study is to assess its effectiveness.
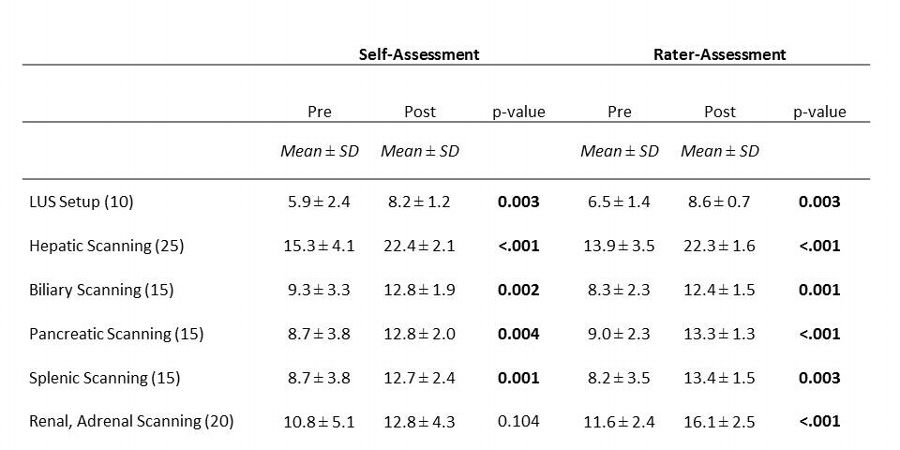
METHODS: Residents rotating on hepatobiliary service dedicated two hours a week to complete the LUS curriculum, consisting of a pre-test, a mentoring session, practice and a post-test. Rater assessment, self assessment and confidence surveys were collected at both intervals. Performance data was obtained using a six component scoring system (table 1.) Comparisons between mean pre- and post-test were performed using the paired t-test.
RESULTS: From 2016-2018, a total of ten surgical residents participated. The self-skills assessment showed a mean increase in total score (58.7±20.4 vs. 81.7±12.6, p=0.001) and all but one component score (Table 1). The rater-skills assessment also showed a mean increase in total score (57.5±10.7 vs. 86.1±5.8, p<.001) and component scores (Table 1). The confidence assessment demonstrated a mean increase in total score (23.0±5.9 vs. 36.7±6.6, p<.001) and in all nine topics after LUS curriculum (all p< .05).
CONCLUSION: Our study demonstrates that a simulation-based laparoscopic ultrasound curriculum during a corresponding rotation increases resident confidence and technical skill. Further studies are needed to assess the transferability to live operative setting.
Table 1.